(Updated post. Please see correction below.)
December is off to a good start for the Nova Scotia Health Authority.
This month it is able to report the first significant decline in the number of citizens who need a family doctor but cannot find one.
5,322 people reported they had found a family doctor and 3,738 registered with NSHA to get help in finding one.
That’s a net improvement of 1,584, the first decline since January. The final number is even better because, beginning this reporting period, NSHA can include results from the Patient Attachment Incentive Trust, which offers docs a one-time payment of $150 for each new patient they take on.
It began April 1 but the results were not counted until now, giving NSHA the benefit of eight months’ of incentives in a single entry.
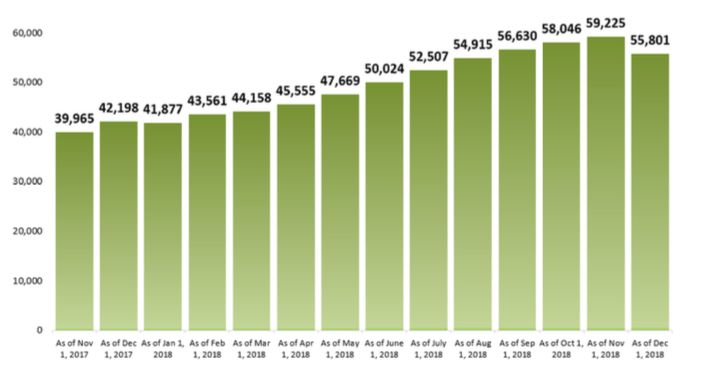
That means there are 55,801 doctor-less citizens as of December 1, down from 59,225 on November 1 (3,424). Whatever number you settle on, it’s a little bit of good news.

And there is more good news at Dartmouth General. The official opening of its new entrance, which faces Acadia Street, happens tomorrow, Dec. 10.
In your correspondent’s view, the “official” opening of a door is a good idea when it’s part of a $140-million renovation because it’s a chance to remind the public this important project is well underway, which makes it harder for governments to stop it.
I say this with the lonely saga of DGH’s ghost floor in mind. It’s the building’s fifth floor, built circa 1988 but left empty until now.
Citizens may recall that during the ghost floor’s big sleep, emergency departments on both sides of Halifax Harbour were practising hallway medicine because there were no beds for emergency patients once they had been stabilized.
This will continue until the construction, finally underway, of the ghostly fifth floor is complete. But it’s galling to know that additional capacity has been available —on the ghost floor— for the last 30 years. It’s the kind of thing that makes voters cynical. Preventing hallway medicine is the responsibility of elected officials and all three political parties have dropped the ball at one time or another.
But enough negativity. The DGH project is itself a part of the much larger “QEII New Generation” project that will replace the VG, Centennial and Dickson buildings in Halifax.
NSHA’s Victoria van Hemert, who is overseeing the whole thing, says the changes at DGH will have a huge impact on the community.
“The big benefit is capacity,” she says. “It means services will be closer to people’s homes.”
Here are some of the other benefits:
- 48 new beds, some of which will accommodate morbidly obese patients
- Renovations are finished on the third and fourth floors.
- Eight new operating rooms (replacing four existing ones), which will increase surgical capacity by 3,500 operations per year.
- Two of the new O.R.’S will be high-volume facilities dedicated to orthopaedic surgery, making DGH a key focus for those procedures.
- Patient rooms will be spacious and offer a view of the outside wherever possible. They will be single-occupancy where feasible. Both features have been proven to speed recovery, reduce relapses and promote infection control.
- Some rooms will have two patients, but that’s the maximum. There will be no four-bed wards.
- Outpatient services capacity (procedures not requiring overnight stays) will double.
- A three-storey addition is under construction and planned for completion next summer. It will house the new O.R.s, a new ambulatory care clinic (ongoing treatments not requiring an overnight stay, such as dialysis), and an endoscopy centre.
The entire project is expected to be finished by late 2021, which pretty much eliminates the possibility of progress being suspended by an election, as it did in 2009 and arguably 2013. This time Premier Stephen McNeil’s government seems to have the bit firmly in its teeth and technically has until 2022 to drop the writ.
Nonetheless, we should keep a sharp eye in the Halifax Infirmary redevelopment, which is ambitious, critical and expensive. Completion might come in 2024-25, which is a long way away in political terms.
NSHA has been refreshingly open about the doctor shortage and the hospital reconstruction. I hope they keep it up and even go further. Believe it or not, open government brings results.
CORRECTION: Earlier, I wrongly reported the fourth floor of Dartmouth General Hospital would be used for administration. It will continue to be an inpatient floor.
-30-
So … you fell for it! Lies, damn lies and statistics in that order. People will continue to die in hallways, para medics will continue the shuttle of the chronically ill between crowded emergencies and spend hours caring for them, families will give up on the search for a GP, qualified medical graduates from away will look elsewhere for opportunities because they can’t afford to pay Dalhousie the fees to enter their territory, Cape Breton will continue to have a high rate of mortality because they can’t serve their patients and can’t send them to Halifax and the rural hospital emergency across the street from us will continue to be closed because there are no staff to support their operation … glad you’re happy! I used to go to the Dartmouth General for diagnostic testing even though at the time it was twice the distance from my home and work than the Victoria General or the QEII. I fail to be impressed but then you were the one who was pissed off because some diagnostic procedures were to be removed from your back yard to Windsor … I remember – “OIMY” (only in my back yard).
LikeLike
Statistics are all we have to measure the doctor shortage and they’re depressing, but I don’t believe NSHA staff are manipulating or lying about them.
And it was Yarmouth, not Windsor. The premier once suggested Haligonians should be prepared to go to Yarmouth for an MRI and I did indeed object to that idea. To be fair, I haven’t heard of him repeating it.
LikeLike